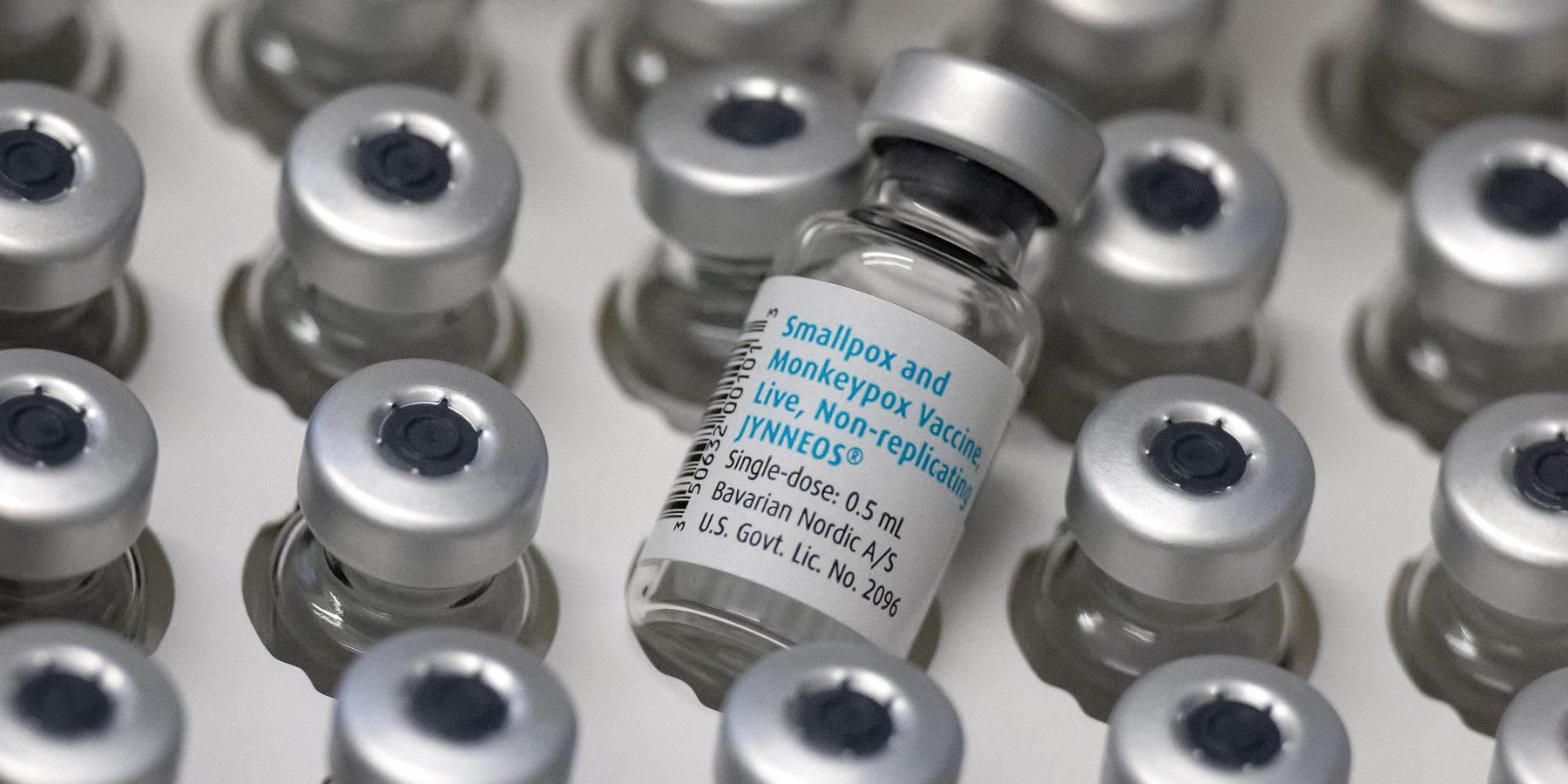
The word, "Monkeypox," did not invade headlines around the globe until recently, but it is not a new disease. Much is known about the virus that originated in Africa, spread among attendees at recent raves in Spain and Belgium, and can lead to serious illness in humans. Below, nine things you should know.
1. It was discovered in 1958 in Denmark by researchers studying monkeys. Monkeys, in fact, are not considered the primary animal-to-human source of the disease. It is more common in rodents.
2. Monkeypox is commonly endemic to certain countries in Sub-Saharan Africa. The Democratic Republic of Congo seems to have the highest burden of disease, but there are fewer than 1,500 cases per year and only about 50 deaths per year. These areas are considered continuously endemic, meaning it is routine for the virus to be found in these areas.
3. There have been multiple prior outbreaks in the United States within the last 20 years. These prior outbreaks seem to be related to exotic pet owners. Random cases have also been reported by people who traveled to some areas of Africa.
4. The disease comes from a virus in the same family as Smallpox, the Orthopoxvirus family, which is why the Smallpox vaccines are useful for both prevention and treatment. To date, there have been 396 cases and no deaths in the United States since January 1.
5. The current outbreak seems to predominantly affect members of the LGBTQIA community, though scientists have said it will be difficult to disentangle whether the current spread was driven by sex or merely close contact. A person’s sexual orientation or gender identity does not put them at higher risk of infection; close contact to an infected person does.
6. Once contracted, the virus is typically asymptomatic for about 10-15 days, then causes five days of fever, chills, muscle aches, headache and fatigue; in general they are flu-like symptoms. After, it has an evolving and painful rash that starts in the groin and buttocks, spreads to the trunk and then to the face. Finally, it can move to the arms.
7. The rash can leave scars. If the rash does not appear, it is not considered Monkeypox. The rash evolves from flat, to fluid-filled, and later pus-filled before falling off and crusting over.
8. Transmission can occur in a variety of ways (in order of most likely to least likely), including bites from infected animals, cleaning animal cages of infected animals, direct human contact with pustules and via respiratory droplets.
9. There are treatment options with vaccines recommended for high risk people, to antivirals, to immunoglobulin treatments and even vaccines given in the post-exposure period. Some people require hospitalization. The CDC recommends isolation for all confirmed cases for at least 21 days after the rash emerges. The CDC and local health departments manage testing.
Dr. Conor Mullin is a board-certified primary care physician specializing in family medicine at University of Michigan Health-West. Dr. Mullin’s practice focuses on family care, primary care, prevention, maternal care, and he is a specialist in LGBTQ+ care including health equity, hormone care, endocrine and transgender care.
Photo via Getty
From Your Site Articles
- 9 Things You Should Know About Monkeypox - PAPER ›
- Jonathan Van Ness Condemns America's "Botched" Monkeypox Response ›
Related Articles Around the Web